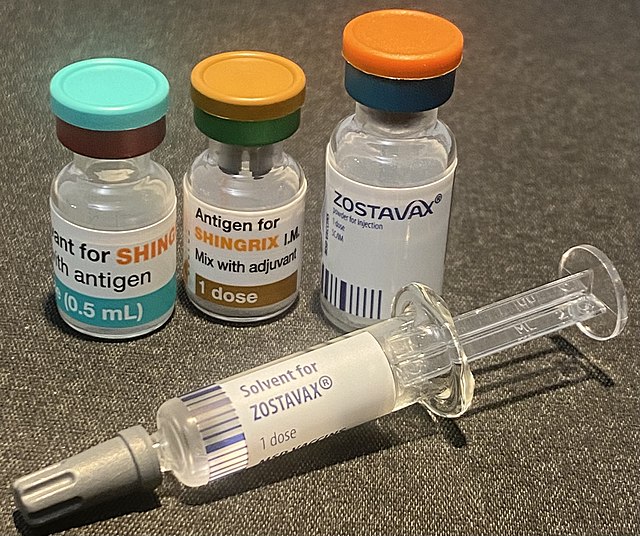
A new study from Wales may offer insight into preventing dementia. Researchers used a new technique which involves an unusual age rule in Wales’ shingles vaccination program to compare two almost identical groups of older adults: those who were allowed to get the vaccine and those who narrowly missed the cutoff.
Because eligibility depended strictly on whether someone turned 80 before or after Sept.1, 2013, scientists could examine people who were essentially the same in every way except for vaccine access. This experiment gave researchers a chance to avoid the problem that people who choose to get vaccinated tend to be more health-conscious than those who do not.
When the team looked at these two groups over several years, their findings were interesting. Those who took the shingles vaccine were about 20% less likely to develop dementia, a finding strongly supported by Stanford Medicine.
The researchers searched for other possible reasons to explain the results, such as differences in education history, prior vaccines taken or underlying and genetic health conditions.
However, no significant differences were found between the suitable and the unsuitable groups. According to Pascal Geldsetzer, the author of the study, “This huge protective signal was there, any which way you looked at the data,” highlighting how consistent the pattern was across all their analyses.
The results add to growing evidence that viruses and the immune system may play a vital role in brain health. Shingles is caused by the varicella-zoster virus, which can remain dormant in the body for a long time.
Some scientists increasingly have a reason to think that viral infections impacting the nervous system could contribute to dementia risk over time.
If stopping shingles infections helps protect the brain, it means that immune responses and viral activity are more connected to cognitive decline than scientists believed.
Researchers found signs that the shingles vaccine might help people who already have dementia. In the follow-up analysis by Stanford Medicine, it was discovered that senior adults with dementia who received the vaccine were significantly less likely to die from the disease over the next nine years.
Almost half of Welsh seniors with dementia eventually died from the condition during the study period, but only about 30% of those who were vaccinated died. This suggests the vaccine might not only slow the development of dementia, but it might also delay its onset.
Researchers are careful to say that a better randomized clinical trial is needed to make a finalized decision. Despite the strength of the Welsh “natural experiment,” only a randomized trial can prove with certainty that the vaccine itself is causing the reduction in dementia risk.
The team hopes the results will motivate funding for such a trial, which would be simple and relatively quick to conduct to determine solid results.
Currently, the findings provide an unexpected and promising possibility that a common vaccine, used widely for shingles, may also help protect the brain.