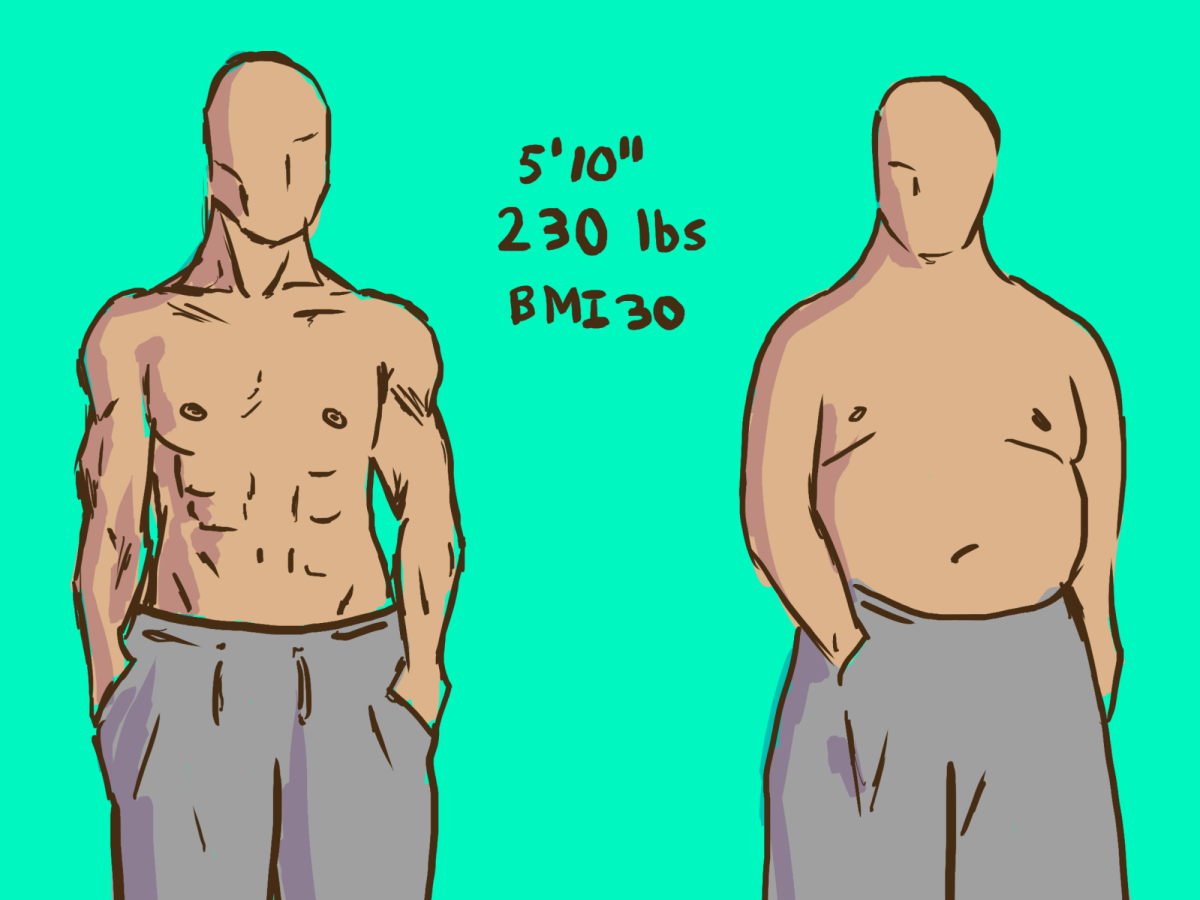
For decades, body mass index has been the go-to metric for defining healthy weight ranges, but its usefulness as a reliable indicator of health is increasingly being questioned.
Originally designed as a simple statistical tool, BMI fails to differentiate between fat and muscle, often misclassifying individuals — particularly athletes and children with higher muscle mass — as overweight or obese.
This one-size-fits-all approach oversimplifies health, ignoring critical factors like body composition, metabolic health and fat distribution.
As a result, many experts have proposed that BMI should not be the sole determinant in assessing obesity or overall well-being.
“[O]besity in adults should not be diagnosed with BMI alone but confirmed with another measure, such as waist-to-height ratio,” the Lancet Commission on Obesity and the European Association for the Study of Obesity said.
Beyond its medical shortcomings, the widespread use of BMI has also had significant psychological consequences, particularly among students.
Children and adolescents, who are already vulnerable to body image concerns, may internalize BMI-based classifications in ways that damage self-esteem and contribute to disordered eating.
A large-scale study followed 7,600 children from ages 9 to 24 and found that of the 1,431 children classified as BMI-overweight at age 9, “64% had waist-to-height ratio normal fat,” meaning they had a normal amount of fat for their weight and height. BMI jumped to a hasty conclusion that these children were unhealthy, without considering the nuances between weight from fat and muscle.
These findings highlight why many researchers support waist-to-height ratio as a more precise measure of adiposity.
“[W]aist-to-height ratio is an affordable and universally accessible, accurate and precise tool for detecting high and excess fat in children and adolescents,” Andrew Agbaje, award-winning physician and associate professor of clinical epidemiology and child health said.
William Dietz, chair of the Sumner M. Redstone Global Center on Prevention and Wellness, has also emphasized BMI’s limitations, explaining that while “BMI is associated with body fat,” it is “not a direct measure of body fat” and “does not assess the concomitant presence of comorbid conditions, disease risks, or functionality.”
He further noted that “BMI’s association with health risk is inconsistent and varies with age, sex, and ethnicity,” and, most importantly, “BMI is not a diagnostic measure of obesity.”
Embracing this approach could help both children and adults receive more accurate health assessments while reducing the stigma and mental toll caused by BMI misclassifications.
Beyond its medical shortcomings, the widespread use of BMI has also had significant psychological consequences, particularly among students.
When schools and healthcare providers place excessive emphasis on BMI without considering broader health markers — such as physical fitness, diet quality and mental health — they risk reinforcing harmful stereotypes about weight.
Shifting toward alternative measures like waist-to-height ratio or body fat percentage would provide a more nuanced and accurate picture of health that prioritizes individual well-being and proportions over arbitrary numerical thresholds. Evidently, relying on BMI as the primary measure of health is an outdated and flawed practice that overlooks other key aspects of an individual’s overall well-being.
The growing body of research advocating for waist-to-height ratio and other alternative metrics underscores the urgent need for a more comprehensive approach to assessing health.
BMI’s limitations not only lead to medical misclassifications but also contribute to the harmful stigma surrounding body weight, particularly among young people. Moving beyond BMI toward more precise and accessible measures will allow for a more accurate understanding of health.
It is time for the medical community to adopt a broader perspective that prioritizes holistic health over rigid, outdated standards.